Introduction
Drinking alcohol is a socially accepted behavior; however, depending on the amount ingested and the pattern of consumption, it could lead to negative health effects that require systematic screening. The spectrum of alcohol use ranges from risky drinking to alcoholism.1
Risky alcohol use (also called binge drinking or heavy drinking) refers to a behavior pattern in which the drinker exceeds certain thresholds that are considered low-risk, whether daily, weekly, or occasionally (i.e., at a meeting, party, or social event).2,3In this regard, the National Institute on Alcohol Abuse and Alcoholism establishes that ideally, alcohol should be limited to a maximum of 3 drinks per day or 7 drinks per week for women, and no more than 4 drinks per day or 14 drinks per week for men.4
According to the World Health Organization (WHO), risky alcohol use causes nearly 3 million deaths each year worldwide,3 and Europe is the region that drinks the most in the world, with 1 in 5 people over the age of 15 years reporting drinking 5 or more alcoholic beverages per occasion at least once a week; this region also has the highest proportion of illness and premature death secondary to alcohol use.5 In the United States, where it is the fourth leading preventable cause of death,6 risky alcohol use has a prevalence of 18.4%,7 a figure similar to that reported in Colombia, where it is 16% for men and 9.1% for women.8 Given this scenario, and taking into account the mortality associated with alcohol use, encouraging a reduction in alcohol use is in line with the sustainable development objective of improving the health and well-being of the population.
Although studies such as the one conducted by Kaner et al.9 demonstrate the effectiveness of brief counseling in reducing alcohol use through primary care, most of the studies on this topic have been conducted in outpatients.9-12
It is well known that risky alcohol use affects health, but there is scant information on this behavior in the hospital population, so a characterization of individuals with this behavior would allow the design of specific intervention strategies. Consequently, the objectives of the present study were to describe the sociodemographic, family, and clinical characteristics of individuals presenting a risky alcohol use behavior and treated at a quaternary care hospital in Bogotá D.C., Colombia, and to evaluate the association between these factors and the intention to reduce alcohol use, measured according to their stage of behavioral change, referred to in this study as "intention to change".
Materials and methods
Study type
Cross-sectional descriptive study conducted based on a randomized clinical experiment carried out between April 2018 and March 202013 to evaluate the effectiveness of brief counseling in modifying risky alcohol and tobacco use behaviors in patients treated at the Hospital Universitario San Ignacio de Bogotá (protocol registered in ClinicalTrials.gov [NCT03521622]).
Study population and sample
All patients between the ages of 19 and 64 years who underwent a surgical intervention or diagnostic procedure at the institution during the study period and in whom risky alcohol use14 and/or active smoking were reported (N=3 609) were considered for the selection of the study population in the original clinical experiment. Subjects were excluded if they had a history of treatment to reduce alcohol use or were under active treatment; if they suffered from diseases that affected their ability to communicate verbally; if they were dependent on or abused alcohol or other psychoactive substances; and if they were in the "action" and "maintenance" stages of behavioral change.15
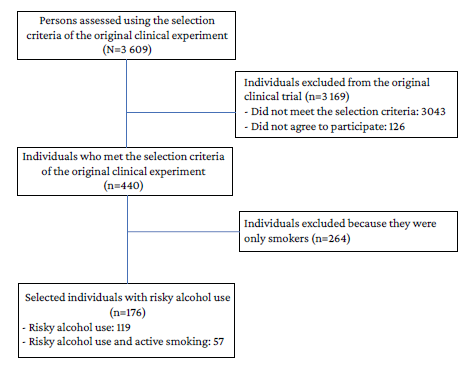
Only individuals with risky alcohol use were considered for sample selection in the present study; thus, 176 participants were included: 119 with risky alcohol use and 57 with risky alcohol use and active smoking. It should be noted that the sample size of the original clinical study was calculated considering progress in behavioral change intention at 1 month and 3 months after brief counseling as the main outcome.13 The sample selection process is described in Figure 1.
Instruments
Risky alcohol use was defined as the consumption of 4 or more standard alcoholic drinks per occasion for women and 5 or more for men during the last 12 months and a score between 8 and 15 on the Alcohol Use Disorders Identification Test (AUDIT), a validated instrument adapted to the Spanish language.14
Sociodemographic characteristics such as age, sex, marital status, socioeconomic level and educational attainment were assessed using questionnaires designed by the authors for this purpose. Regarding family characteristics, the Apgar family questionnaire16 was used to identify family structure, family life cycle, and family functionality. Direct interviews with the participants were conducted to inquire about the presence of clinical comorbidities (with emphasis on chronic diseases) and the coexistence of smoking as a risk factor, the latter defined as the use of any tobacco-containing product during the last month and smoking more than 100 cigarettes over the course of one's life.
Finally, aspects related to alcohol use, such as motivation to change drinking behavior (desire to reduce risky alcohol use), perceived self-efficacy (individual's perceived likelihood of achieving change if they made the effort to do so) and attempts to change, were measured using analogous scales (scores from 1 to 10) and patient self-reporting by means of a structured interview. Measurements of the characteristics of the included population were taken at the initial or "baseline" time of the original clinical trial.
Procedures
The dependent variable in the present study was denominated intention to change; it considers the existence of phases or stages in the process of behavioral change known as Precontemplation, Contemplation, and Preparation. The instrument used for its measurement was the Spanish version of the Readiness to Change Questionnaire, a 12-item instrument validated in Spanish based on the stages of change proposed by Prochaska and DiClemente in 1986, which provides three 4-item scales, each representing one of the previously mentioned stages of change.17
Information was collected during the patients' stay in the hospital and by means of the electronic data capture system REDCap version 7.3.6.18
Statistical analysis
The data were analyzed using the R software version 4.0.3. The variables evaluated were categorized, and absolute frequencies and proportions were calculated. The prevalence of risky alcohol use was determined taking into account the number of participants who met this definition over the total number of subjects assessed with the selection criteria in the original clinical experiment (subjects with risky alcohol use/total number of subjects assessed).
A bivariate analysis was performed to identify possible associations between independent variables (sociodemographic, family, and clinical variables) and the dependent variable (intention to change), using the chi-square test, with a significance value of p<0.05. Furthermore, a multivariate analysis was performed by means of an ordinal logistic regression in which variables with a significant association in the bivariate analysis (p<0.05) were included, calculating adjusted Odd Ratios (aOR) with their corresponding 95% confidence intervals (95%CI) and a significance level of p<0.05.
Ethical considerations
The study took into account the ethical principles for research involving human subjects established in the Declaration of Helsinki19 and the health research provisions of Resolution 8430 of 1993 of the Colombian Ministry of Health.20 The original clinical trial was also approved by the Institutional Research and Ethics Committee, which comprises members of the Hospital Universitario San Ignacio and the Pontificia Universidad Javeriana, according to Minutes No. FM-CIE-0025-18 of January 25, 2018. All participants independently and voluntarily signed the informed consent form.
Results
The prevalence of risky alcohol use was 4.88% (95%CI: 4.17-5.58), a percentage that represents the population included in this study out of the total population assessed using the selection criteria of the original clinical trial (176/3 609).
Regarding the sociodemographic characteristics of the participants, it was found that the majority were men (83.95%), over 45 years of age (39.20%), married or living in cohabitation (48.29%), came from a low (55.68%) or middle (41.47%) socioeconomic level, and had primary or high school education as their highest educational level (58.52%). Concerning family characteristics, it was found that 59.09% had a family with a nuclear structure, that the most frequent stage of the family life cycle was the launching stage (36.93%), and that the majority rated their family functionality as adequate (58.52%). Finally, referring to clinical characteristics, it was established that the majority of participants (56.25%) did not have chronic diseases (Table 1).
Table 1 Characteristics of participants with risky alcohol use assessed at the Hospital Universitario San Ignacio, Bogotá D.C., Colombia.
| Characteristics | Total (n=176) | % | ||
|---|---|---|---|---|
| Demographic characteristics | Sex | Male | 146 | 82.95 |
| Female | 30 | 17.05 | ||
| Age | 19-30 years | 51 | 28.97 | |
| 31-45 years | 56 | 31.81 | ||
| 46-64 years | 69 | 39.22 | ||
| Marital status | Single | 79 | 44.89 | |
| Divorced | 12 | 6.82 | ||
| With a partner | 85 | 48.29 | ||
| Socioeconomic level | Low (1 and 2) | 98 | 55.68 | |
| Middle (3 and 4) | 73 | 41.48 | ||
| High (5 and 6) | 5 | 2.84 | ||
| Educational attainment | Basic/intermediate (elementary school/high school) | 103 | 58.52 | |
| Higher (technical/university) | 64 | 36.36 | ||
| Postgraduate | 9 | 5.11 | ||
| Family characteristics | Family type | Nuclear | 104 | 59.09 |
| Extensive | 16 | 9.09 | ||
| Composite | 10 | 5.68 | ||
| One-person | 22 | 12.50 | ||
| Another | 24 | 13.64 | ||
| Family cycle | Beginning/developing | 46 | 26.14 | |
| Launching stage | 65 | 36.93 | ||
| Post-parental | 14 | 7.95 | ||
| Dissolution | 13 | 7.39 | ||
| Not classifiable/Not applicable | 37 | 21.02 | ||
| No data | 1 | 0.57 | ||
| Family functionality (Apgar) | Good functionality (18-20 points) | 103 | 58.52 | |
| Dysfunctional (≤17) | 71 | 40.34 | ||
| No data | 2 | 1.14 | ||
| Clinical characteristics | Associated chronic diseases | Yes | 76 | 43.18 |
| No | 99 | 56.25 | ||
| No data | 1 | 0.57 | ||
Source: Own elaboration.
Regarding the characteristics of risky alcohol use, more than half (60.22%) of the participants had a score between 8 and 11 on the AUDIT test and reported making an attempt to reduce its use at some point in their lives. Concerning participants' attitude towards reducing alcohol use, most of them had a high perception of the benefits that this could bring them (91.48%) and were placed on a high scale of motivation (91.48%); likewise, 162 (92.05%) patients reported feeling capable of reducing their exposure to this risk factor. With respect to the stage of behavioral change in which the participants were in concerning alcohol use reduction, the majority were in the Preparation stage (63.64%), followed by the Contemplation (25.57%), and Precontemplation (10.79%) stages (Table 2).
Table 2 Characteristics related to risky alcohol use among the participants assessed at the Hospital San Ignacio, Bogotá D.C., Colombia.
| Characteristics | Total (n=176) | % | ||
|---|---|---|---|---|
| Risky behavior | Risky alcohol use | 119 | 67.61 | |
| Smoking and risky alcohol use | 57 | 32.39 | ||
| Total AUDIT score | 8-11 | 106 | 60.23 | |
| 12-15 | 70 | 39.77 | ||
| Attitude towards risky behavior | Perception of benefit | Low (≤5/10) | 15 | 8.52 |
| High (>5/10) | 161 | 91.48 | ||
| Motivation level | Low (≤5/10) | 15 | 8.52 | |
| High (>5/10) | 161 | 91.48 | ||
| Self-efficacy | Low (<5/10) | 14 | 7.95 | |
| High (>5/10) | 162 | 92.05 | ||
| Attempts to reduce alcohol use | Yes | 110 | 62.50 | |
| No | 66 | 37.50 | ||
| Number of previous attempts (n=110) | 1-5 times | 81 | 73.64 | |
| ≥6 times | 29 | 26.36 | ||
| Stage of change | Preparation | 112 | 63.64 | |
| Contemplation | 45 | 25.57 | ||
| Precontemplation | 19 | 10.79 | ||
AUDIT: Alcohol Use Disorders Identification Test.
Source: Own elaboration.
In the bivariate analysis, it was established that most participants were in the Preparation stage (n=112), with a higher percentage of men (67.80% vs. 43.33%), this difference being statistically significant (p=0.016). Likewise, being from the low and middle socioeconomic levels was significantly associated with having a higher intention to change compared to the upper levels (p=0.047) (Table 3).
Table 3 Factors associated with intention to change among participants with risky alcohol use assessed at the Hospital San Ignacio, Bogotá D.C., Colombia.
| Characteristics | Stage of behavioral change | ||||||
|---|---|---|---|---|---|---|---|
| Precontemplation (n=19) | Contemplation (n=45) | Preparation (n=112) | Total (n=176) | Valorp | |||
| Demographic characteristics | Sex | Male | 7 (23.33%) | 10 (33.33%) | 13 (43.33%) | 30 (17.05%) | 0.016 |
| Female | 12 (8.21%) | 35 (23.97%) | 99 (67.81%) | 146 (82.95%) | |||
| Age | 19-30 years | 9 (17.65%) | 18 (35.29%) | 24 (47.06%) | 51 (28.98%) | 0.062 | |
| 31-45 years | 5 (8.93%) | 11 (19.64%) | 40 (71.43%) | 56 (31.82%) | |||
| 46-64 years | 5 (7.25%) | 16 (23.19%) | 48 (69.56%) | 69 (39.20%) | |||
| Marital status | Married or in a domestic partnership | 8 (9.41%) | 23 (27.06%) | 54 (63.53%) | 85 (48.29%) | 0.74 | |
| Single | 11 (13.92%) | 19 (24.05%) | 49 (62.02%) | 79 (44.89%) | |||
| Divorced | 0 (0.00%) | 3 (25.00%) | 9 (75.00%) | 12 (6.82%) | |||
| Socioeconomic level | Low (1 and 2) | 11 (11.22%) | 25 (25.51%) | 62 (63.26%) | 98 (55.68%) | 0.047 | |
| Middle (3 and 4) | 5 (6.85%) | 20 (27.40%) | 48 (65.75%) | 73 (41.48%) | |||
| High (5 and 6) | 3 (60.00%) | 0 (0.00%) | 2 (40.00%) | 5 (2.84%) | |||
| Educational attainment | Basic/intermediate (elementary school/high school) | 7 (6.80%) | 28 (27.18%) | 68 (66.02%) | 103 (58.52%) | 0.13 | |
| Higher (technical/university) | 9 (14.06%) | 16 (25%) | 39 (60.94%) | 64 (36.36%) | |||
| Postgraduate | 3 (33.33%) | 1 (11.11%) | 5 (55.55%) | 9 (5.11%) | |||
| Family characteristics | Family type | Nuclear | 12 (11.54%) | 29 (27.88%) | 63 (60.58%) | 104 (59.09%) | 0.94 |
| Extensive | 2 (12.50%) | 3 (18.75%) | 11 (68.75%) | 16 (9.09%) | |||
| Composite | 2 (20.00%) | 2 (20.00%) | 6 (60.00%) | 10 (5.68%) | |||
| One-person | 1 (4.54%) | 5 (22.72%) | 16 (72.73%) | 22 (12.50%) | |||
| Another | 2 (8.33%) | 6 (25.00%) | 16 (66.66%) | 24 (13.64%) | |||
| Family cycle | Beginning/developing | 8 (17.39%) | 12 (26.09%) | 26 (56.52%) | 46 (26.14%) | 0.84 | |
| Launching stage | 5 (7.69%) | 17 (26.15%) | 43 (66.15%) | 65 (36.93%) | |||
| Post-parental | 1 (7.14%) | 4 (28.57%) | 9 (64.28%) | 14 (8.00%) | |||
| Dissolution | 0 (0.00%) | 2 (15.38%) | 11 (84.61%) | 13 (7.39%) | |||
| Not classifiable/Not applicable | 4 (10.81%) | 10 (27.03%) | 23 (62.16%) | 37 (21.02%) | |||
| No data | 1 (100.00%) | 0 (0.00%) | 0 (0.00%) | 1 (0.57%) | |||
| Family functionality (Apgar) | Good functionality (18-20 points) | 12 (11.65%) | 18 (17.47%) | 73 (70.87%) | 103 (58.52%) | 0.01 | |
| Dysfunctional (<17) | 6 (8.45%) | 27 (38.03%) | 38 (53.52%) | 71 (40.34%) | |||
| No data | 1 (50.00%) | 0 (0.00%) | 1 (50.00%) | 2 (1.14%) | |||
| Clinical characteristics | Associated chronic diseases | Yes | 6 (7.89%) | 20 (26.31%) | 50 (65.79%) | 76 (43.18%) | 0.58 |
| No | 13 (13.13%) | 24 (24.24%) | 62 (62.63%) | 99 (56.25%) | |||
| No data | 0 (0.00%) | 1 (100.00%) | 0 (0.00%) | 1 (0.57%) | |||
| Risky behavior | Risky alcohol use | 12 (10.08%) | 31 (26.05%) | 76 (63.86%) | 119 (67.61%) | 0.94 | |
| Smoking and risky alcohol use | 7 (12.28%) | 14 (24.56%) | 36 (63.16%) | 57 (32.39%) | |||
| Total AUDIT score | 8-11 | 13 (12.26%) | 20 (18.87%) | 73 (68.87%) | 106 (60.23%) | 0.045 | |
| 12-15 | 6 (8.57%) | 25 (35.71%) | 39 (55.71%) | 70 (39.77%) | |||
| Attitude towards risky behavior | Perception of benefit | ≤5/10 | 7 (46.67%) | 4 (26.67%) | 4 (26.67%) | 15 (8.52%) | 0.0001 |
| >5/10 | 12 (7.45%) | 41 (25.46%) | 108 (67.08%) | 161 (91.48%) | |||
| Level of motivation | ≤5/10 | 7 (46.67%) | 5 (33.30%) | 3 (20.00%) | 15 (8.52%) | 0.0001 | |
| >5/10 | 12 (7.45%) | 40 (24.84%) | 109 (67.70%) | 161 (91.48%) | |||
| Self-efficacy | <5/10 | 4 (28.57%) | 5 (35.71%) | 5 (35.71%) | 14 (7.95%) | 0.03 | |
| >5/10 | 15 (9.26%) | 40 (24.69%) | 107 (66.05%) | 162 (92.04%) | |||
| Attempts to reduce alcohol use * | No | 11 (16.67%) | 22 (33.33%) | 33 (50.00%) | 66 (37.50%) | 0.01 | |
| Yes | 8 (7.27%) | 23 (20.91%) | 79 (71.82%) | 110 (62.50%) | |||
| Number of attempts | 1-5 times | 7 (8.64%) | 18 (22.22%) | 56 (69.13%) | 81 (73.64%) | 0.15 | |
| ≥6 times | 1 (3.45%) | 5 (17.24%) | 23 (79.31%) | 29 (26.36%) | |||
AUDIT: Alcohol Use Disorders Identification Test.
* Values for this variable were calculated from the sample of individuals who reported that they had made previous attempts to reduce alcohol use (n=110).
Source: Own elaboration.
With respect to family characteristics, good family functionality was correlated with a higher intention to change compared to having some degree of family dysfunction (p=0.01).
When analyzing variables related to intention to change, the proportion of patients who were in the Preparation stage was higher among those with lower AUDIT scores than among those with higher scores (68.87% vs. 55.71%; p=0.045). On the other hand, high scores on perceived benefits (p=0.0001), degree of motivation (p=0.0001) and self-efficacy (p=0.03) were significantly associated with greater progress in intention to change. The variable with the strongest association was level of motivation, finding that lower motivation was related to a higher percentage of subjects in the Precontemplation stage (p=0.0001) compared to those with higher reported motivation, who were in more advanced stages concerning their intention to change (Table 3). Moreover, previous attempts to reduce alcohol use were significantly associated with higher current intention to change (p=0.01) (Table 3).
The multivariate analysis found a significant association between age and greater intention to change. In this sense, being between 31 and 64 years of age was associated with a higher probability of intention to change (aOR=3.68; 95%CI: 1.56-9.06 for 31 to 45 years, and aOR=2.63; 95%CI: 1.20-5.86 for 46 to 64 years), compared to the group aged 19 to 30 years. Additionally, being from a high socioeconomic level was associated with a lower intention to change (aOR=0.06; 95%CI: 0.01-0.50) (Table 4).
With respect to variables related to attitude towards alcohol use assessed using verbal self-report scales, having a high perception of benefit (score between 6 and 10) and feeling more capable of modifying the risk factor (self-efficacy) were associated with a higher intention to change (aOR=7.32; 95%CI: 2.46-23.19 and aOR =3.08; 95%CI: 1.01-9.38, respectively) (Table 4).
Finally, having at least one previous attempt to reduce alcohol use was associated with a higher intention to change (aOR=2.02; 95%CI: 1.02-3.99) (Table 4).
Table 4 Factors associated with intention to change among individuals with risky alcohol use.
| Characteristics | Adjusted OR | 95%CI | ||
|---|---|---|---|---|
| Demographic characteristics | Sex | Male | 2.19 | 0.96-4.96 |
| Age | 31-45 years | 3.68 | 1.56-9.06 | |
| 46-64 years | 2.63 | 1.20-5.86 | ||
| Socioeconomic level | Middle (3 and 4) | 1.36 | 0.69-2.73 | |
| High (5 and 6) | 0.06 | 0.01-0.50 | ||
| Attitude towards risky behavior | Perception of benefit | >5/10 | 7.32 | 2.46-23.19 |
| Self-efficacy | High (>5/10) | 3.08 | 1.01-9.38 | |
| Attempts to reduce alcohol use | Yes | 2.02 | 1.02-3.99 | |
Source: Own elaboration.
Discussion
Early intervention of risky alcohol use helps to reduce premature deaths and disability from this cause worldwide. Several studies have described the effectiveness of brief interventions aimed at reducing this risk, which can be initiated in both outpatient and inpatient settings.1,12,21-24
In Colombia, there is scant information on the prevalence of risky alcohol use in hospital settings among individuals without a diagnosis of a disease related to the consumption of this substance. Nevertheless, the present study provides information on the demographic, family and clinical characteristics of a group of drinking subjects and their association with the intention to change, and the results obtained allow identifying variables that could be used by health professionals as markers of good prognosis for the implementation of brief interventions aimed at reducing alcohol use.
The prevalence of risky alcohol use in the present study (4.88%) was near to, but lower than, the prevalence reported for the general Colombian population in the 2019 National Study of Psychoactive Substance Use, in which this figure was 6.1%.25 The lower prevalence found here may be explained by the fact that the subjects included had some medical condition that led to the performance of diagnostic studies or surgeries (which may have affected their current alcohol use) and that the majority of participants were over 30 years of age (71%), in whom alcohol consumption is lower compared to younger people.25
The distribution of demographic and clinical variables among the population analyzed in the present study has similarities with other populations treated at tertiary care hospitals and with the trends of risky alcohol use in the general population:8 of the total number of patients with risky alcohol use, most were men (82.95%), had a partner (48.29%), came from a low socioeconomic level (55.68%), and had a low educational attainment (58.52%), which is similar to the characteristics documented for this type of population in Colombia by the National Government.25
Bivariate analysis suggested that having good family functionality is associated with greater intention to change (p=0.01). In this regard, it has been described that not having family support or being away from the family are emotional risk factors that may favor the use of alcohol and other psychoactive substances. In the particular case of the Hispanic population, Caetano et al.,26 through a study conducted in a random sample of 1 510 Puerto Rican adults (18 to 64 years old), reported that low and moderate family cohesion, defined as the bonding bridge that family members have with each other, is related to a higher probability of having a diagnosis of alcohol use disorder (aOR=2.20, 95%CI: 1.21-3.98; p<0.01, and aOR=1.88; 95%CI: 1.12-3.14; p<0.01, respectively). In turn, family relationships become negative and problematic when there is a member who suffers from alcohol abuse, which can cause the family to disintegrate27 or alter the roles and functions of each member.28
Age, socioeconomic level, and variables concerning the subject's attitude towards alcohol use (perceived benefits and self-efficacy, and previous attempts) were significantly associated with intention to change in the multivariate analysis. In relation to age, the finding of a higher intention to change in subjects older than 30 years (aOR=3.68, 95%CI: 1.56-9.06 for 31 to 45 years, and aOR=2.63, 95%CI: 1.20-5.86 for 46 to 64 years) is consistent with what has been reported in the literature worldwide. Studies carried out in Spain,29 the United Kingdom,30 and Australia31 have documented that adolescents, young people and/or university students have a higher prevalence of alcohol use and an underestimation of risky alcohol use, both in the short and long term. This is associated with positive reinforcement in the social environment, the management of negative emotions through alcohol, and the immediate feeling of well-being produced by this substance.24
Furthermore, the present study identified an inverse association between socioeconomic level and intention to change, showing that individuals from higher socioeconomic levels are less likely to reduce their consumption compared to those from lower socioeconomic levels (ORa=0.06; 95%CI: 0.01-0.50). In Colombia, the consumption of alcoholic beverages has been found to be more frequent among individuals in higher socioeconomic levels, but data from the 2019 National Study of Psychoactive Substance Consumption indicate that the negative effects of alcohol and the prevalence of risky use patterns are more significant in lower socioeconomic levels.25 The foregoing generates an inverse distribution; that is, in the lower levels (1 and 2) consumption is less frequent but consumption patterns are riskier, while in the higher levels, consumption is more frequent but it occurs in smaller quantities.8,25The latter may be related to a lower perception of the risk of harmful alcohol use and, therefore, to a lower intention to change, which is consistent with the findings of the present study.
On the other hand, the perceived health benefits of reducing alcohol use was the factor that had the strongest association with the intention to change (aOR=7.32; 95%CI: 2.46-23.19). Also, the perception of being able to modify the behavior, i.e., self-efficacy, and previously attempting to reduce consumption were associated with a higher intention to change (aOR=3.08, 95%CI: 1.01-9.38 and aOR=2.02, 95%CI: 1.02-3.99, respectively). These results may be related to the fact that a greater knowledge of risks and, therefore, a greater desire to work on self-care are associated with a higher likelihood of changing. In this regard, the WHO32 states that the timely identification of this phenomenon and the implementation of brief interventions tailored to each subject could promote greater awareness of harm, hence brief interventions are desirable to reduce risky alcohol use.
With respect to self-efficacy, it has been described that people who consider that they have this ability are more likely to modify their intention to change than those who do not.9 This is supported by Bandura's theory of self-efficacy, which, according to Quilas-Benites et al.,33 refers to a key personal factor for achieving behavioral change, since it provides a mechanism through which people demonstrate control over their own motivations and actions. Self-efficacy is even considered as a predictor of alcohol reduction treatment outcomes.34 In this sense, brief interventions are effective in generating behavioral changes, as they help empower people and establish a concrete goal, given that they perceive themselves as capable of achieving their specific objective.35
In view of the aforementioned, promoting attempts to change is a crucial step to achieve long-term effects regarding alcohol use reduction.36 Thus, having previous attempts to reduce consumption gives the person the confidence of being successful in reducing consumption in the past and, aware of this, makes them feel more prepared to achieve a long-term reduction.36 Therefore, it should be kept in mind that attempts to cease a negative behavior, whether successful or not, promote strength and increase self-efficacy.37
The main limitation of the present study was the fact that data on participants' alcohol use were obtained through self-reporting and were not confirmed objectively. Accordingly, it cannot be ruled out that being in the perioperative period or in the process of undergoing diagnostic studies for different diseases may have influenced participants' responses.
Conclusions
In the present study, most individuals who consumed alcohol at risky levels were male, had no comorbidities, were married or cohabiting, had a basic level of education, came from middle and low socioeconomic levels, and belonged to nuclear families on the launching stage and had an adequate functionality. Likewise, a statistically significant association was found between intention to change and being older than 30 years, having a high perception of health benefits after reducing alcohol use, a high perception of self-efficacy, and previous attempts to reduce alcohol use. On the contrary, belonging to a higher socioeconomic level was associated with a lower intention to change.
The identification of variables that favor the change of a risk behavior, such as risky alcohol use, can contribute to the design of brief counseling interventions adjusted to the hospital setting; in addition, these variables can be used as a good prognostic marker for the reduction of the burden of disease associated with the occurrence of chronic diseases. In this regard, screening and treatment of alcohol use in all health care delivery settings, including the hospital setting, is a priority.