Introduction
The giant colonic diverticulum (GCD) is a rare clinical entity, with fewer than 200 reported cases1; it was first described in 1946 by Bouvin and Bonet2,3. It is a lesion originating from the antimesenteric border; the sigmoid is the most frequent site of manifestation. The size fluctuates between 4 and 30 cm, and they are generally simple and single lesions, but they can be multiple, considered an infrequent manifestation of colonic diverticulosis3. Among the reported complications are perforation, abscess, volvulus, infarction, and adenocarcinoma3,4. Segmental colectomy is regarded as the ideal treatment or diverticulectomy when the giant diverticulum is single5. We present this entity’s case in a male patient in the fifth decade of life.
Case presentation
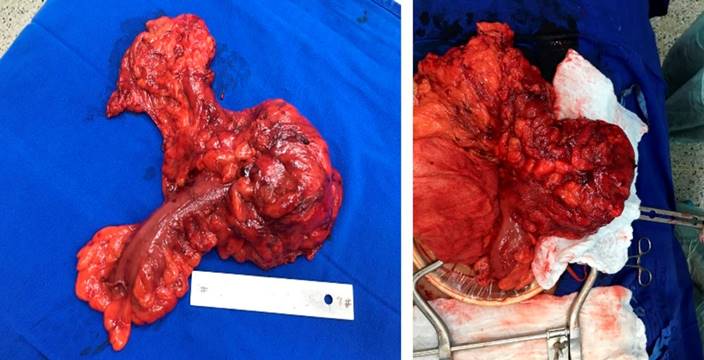
This is the case of a 42-year-old male patient with no relevant pathological history. The patient initially consulted due to a two-year history of pain in the left hemiabdomen, associated with a sensation of mass and intestinal habit with periods of constipation and diarrhea. He made multiple consultations in which he was medically treated without improvement. A colonoscopy was performed on an outpatient basis with poor colonic preparation due to fecal matter at the rectosigmoid junction. Double-contrast computed tomography (CT) of the abdomen reported dolichosigma and occupation of the colon-sigmoid junction with hypodense and heterogeneous material that reached a transverse diameter of 8 cm, giving rise to the suspicion of segmental fecal impaction in front of a bezoar. A control CT scan (Figure 1) was performed at Hospital Universitario San Ignacio, the findings of which suggested a bezoar in the lumen of the distal descending colon, not associated with intestinal obstruction, as the first possibility. He was assessed for colon and rectal surgery and considered a patient with a giant diverticulum in the descending colon, for which resection and anastomosis by laparotomy were prioritized. The intraoperative findings (Figure 2) showed a rounded lesion in the descending colon, towards the lateral edge of the antimesenteric surface, 10 x 8 cm, with a soft consistency. There were no postoperative complications, and he was discharged on day seven.
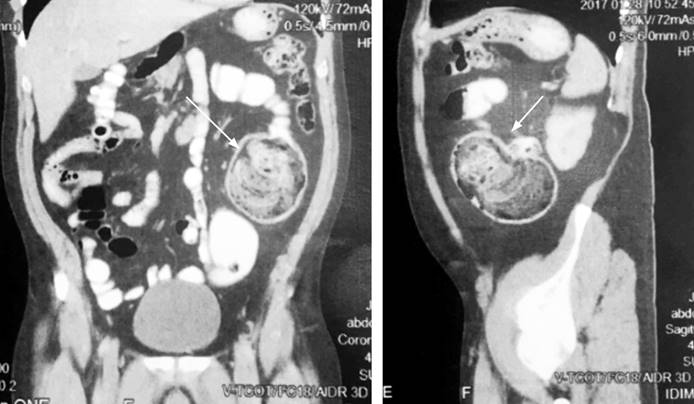
Figure 1 CT with double contrast, coronal and sagittal section (lesion indicated by the arrow). Source: Patient’s medical record.
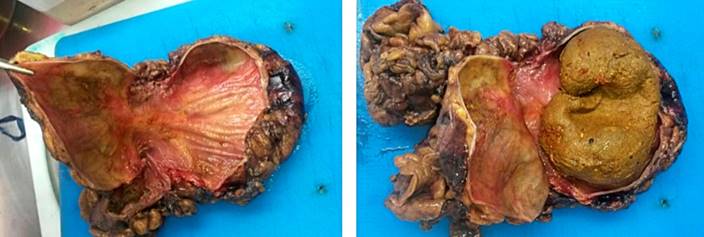
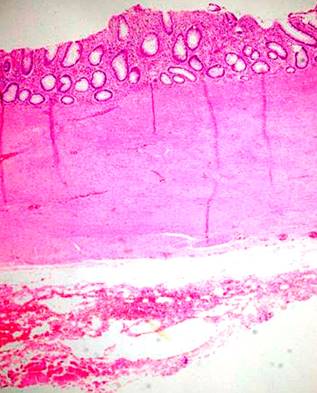
In the anatomopathological findings, a large diverticulum with a small mouth is macroscopically described but with a cavity of 8.3 x 5 cm; when cut, abundant fecal content was found without perforations or masses (Figure 3). The microscopic diagnosis confirms a diverticular formation (Figure 4), with all the layers in the wall of the diverticulum corresponding to a true giant diverticulum.
Discussion
Colonic diverticula are herniations of the mucosa and muscular layer of the mucosa through a weakness in the muscular wall, where the arteries penetrate it4,6. These diverticula are usually of constant size and range between 0.5 and 1 cm in diameter4. These diverticular formations are considered false diverticula because they do not have all the typical layers of the gastrointestinal tract. Diverticula can be found throughout the entire colon. Still, in most cases, diverticular disease is located in the sigmoid colon4, where diverticula average between 1 and 2 cm in size, in contrast to sigmoid diverticula, which are acquired and usually multiple5.
Colonic diverticulosis is a common pathology in Western countries, mainly attributed to the low fiber intake in the diet7. The prevalence increases with age from the fourth decade onwards and is very frequent in advanced ages, affecting up to 70% of individuals in the seventh decade of life, mainly men4. This pathology is usually asymptomatic, but it can become complicated, and the most common is acute diverticulitis in 15% to 30% of patients with colonic diverticulosis, followed by bleeding2,3,8.
GCD is a rare but well-known variant, defined as a diverticulum larger than 4 cm. 85% of GCDs are associated with diverticular disease9, and 90% of these diverticula are located on the antimesenteric edge. They are generally simple and single but can be multiple4; their size fluctuates between 4 and 30 cm. It occurs more frequently between 60 and 80 years; however, it can be found in the age range between 38 and 86 years, both in men and women1,2,10.
Clinically, the manifestation may vary. Abdominal pain is the most common symptom in 69% of cases, followed by constipation10, sensation of abdominal mass, vomiting, rectal bleeding, and fever in up to 20% of cases; even so, the literature subdivides them into four clinical groups3,9,10:
Acute (30%-35%): Abdominal pain, fever, symptoms and signs of intestinal obstruction, and rectal bleeding.
Chronic (35%): It occurs in one-third of patients and has nonspecific symptoms, such as abdominal discomfort, bloating, and constipation.
Complicated (10%-20%): It occurs in 6% of patients as an acute abdomen secondary to perforation, abscess, volvulus, urinary or intestinal obstruction, infarction, and even fistula formation, and extremely rarely, the appearance of adenocarcinoma within the GCD.
Asymptomatic (10%): It is detected as a mass on physical examination or as an incidental finding on imaging, in which a differential diagnosis should be made with other entities that appear as a cavity filled with air or with air-fluid levels such as volvulus, duplication cysts, duodenal diverticula, Meckel’s diverticulum, abscesses, necrotic tumors, or emphysematous cholecystitis.
The most accepted pathogenic theory refers to a ball valve mechanism through which gas enters but cannot exit the diverticulum. The unidirectional air passage produces pressure elevation and pressure differences in the colon, with the gradual enlargement of the diverticulum2.
Given the diagnostic suspicion of this entity, the test of choice is double contrast tomography. Typically, a round gas-filled structure is described with or without a hydro-aerial level2. Colonoscopy frequently does not diagnose because the orifice of the diverticular neck can be hermetic to allow viewing, and contrast enemas can demonstrate communication of the diverticulum with the intestinal lumen in almost 70% of cases; however, recent publications suggest that the barium enema should be avoided due to the risk of perforation11.
The histological classification proposed by McNutt in 1988 is still valid to this day. This classification subdivides GCD into three subtypes: pseudodiverticulum, inflammatory, and true or congenital, each with different microscopic characteristics2.
The treatment of GCD depends on its clinical classification1. For uncomplicated and symptomatic GCD, it is primary resection of the diverticulum with margins and primary anastomosis. In the case of an acute abdomen secondary to perforation and peritonitis, the safest treatment is en bloc resection of the diverticulum and the affected colon associated with a terminal temporary colostomy.
Conclusion
The true giant diverticulum of the colon is a rare entity. We presented the clinical case of a patient who consulted on several occasions due to abdominal pain symptoms interpreted as irritable bowel syndrome, studied with colonoscopy and CT in which a lesion in the distal descending colon was finally documented. He underwent an exploratory laparotomy where a left hemicolectomy with colocolonic anastomosis was performed without complication. A mass was identified at the descending colon level corresponding to a fecaloma originating from a true giant diverticulum of the colon. Giant diverticula have been described in the context of diverticulosis in various colon segments. However, a true diverticulum at this level makes it a rare finding since they are mainly detected in the right colon, while pseudodiverticula are usually reported in the left colon. As noted in the reviewed literature, the treatment given to this patient is adequate; despite being a rare pathology, it should be considered a differential diagnosis given the possible complications that may arise.











 texto en
texto en