INTRODUCTION
The Herlyn-Werner-Wünderlich syndrome (HWW), also known as OHVIRA - obstructed hemivagina and ipsilateral renal agenesis- is the association of a series of urogenital anatomical alterations classified within the Müllerian pathologies. It is characterized by renal agenesis, uterus didelphys and complete or incomplete vaginal obstruction, predominantly on the right side. 1 These abnormalities often cause in patients dysmenorrhea, abnormal vaginal discharges, endometriosis, pyosalpinx, hematometra, hematocolpos, pyometra and pyocolpos.
Its etiopathology is not clear; however, when Müllerian ducts fuse, the uterus, cervix and vaginal dome are formed, so a deficit in their union explains the genital malformations. 2 Furthermore, the Wolf duct, which has a mesoderm origin, is poorly developed, affecting the embryogenesis of the kidney and the ipsilateral ureter, among other malformations of the urinary system. 3
CASE PRESENTATION
A female 17-year-old patient, from the department of Casanare, Colombia, and of mixed race, visited the gynecological and obstetric emergency department for the first time due to strong acute abdominal pain in the hypogastric region and iliac fossae of one hour evolution (VAS 8/10), which did not irradiate, was not related to any activity or food consumption, and presented with slight foul-smelling vaginal bleeding. There was no evidence of emesis or diaphoresis nor was it related to febrile peaks.
The young woman did not report any pathological, family, surgical, allergic or pharmacological history or toxic habits. Menarche occurred at 12 years of age with irregular menstrual cycles, having the last menstrual period 3 months before the consultation; her first sexual intercourse occurred at age 16, stating that her sexual relations have been pleasant without pregnancies. The patient manifested using levonorgestrel subdermal implants for 5 months for birth control, which could be related to oligomenorrhoea symptoms.
Physical examination revealed normal heart and breathing rates, as well as temperature and blood pressure within normal ranges for physical body and age. The abdomen was not distended and no signs of peritoneal irritation were found; however, the patient felt pain on deep palpation in the right iliac fossa and hypogastrium. During the gynecological examination, the woman showed significant pain, making exploration difficult.
Considering the symptoms, pregnancy or infection of the urogenital tract were suspected; paraclinical results showed negative pregnancy test, blood count with leukocytosis without neutrophilia (leukocytes 15 300 and neutrophils 61.6%), without anemia (hemoglobin 14.2 gr/L, hematocrit 41%) and platelets 433 000/uL. Urinalysis did not suggest urinary tract infection. Transvaginal ultrasound and abdominal pelvic tomography were requested, revealing uterus didelphys (Figure 1) and renal agenesis (Figure 2).

Source: Document obtained during the study.
Figure 1 Transvaginal gynecology ultrasound showing the presence of uterus didelphys (demarcated in yellow).

Source: Document obtained during the study.
Figure 2 Coronal computed tomographic (CT) scan that shows the left kidney and right renal agenesis.
Reassessment was performed after pain decreased with the administration of analgesics; speculation was performed, and hematopurulent discharge was observed after draining using a continuity solution of 1mm to 2 mm in length in the vaginal transverse septum, which documented hematopyometra.
Antibiotic treatment was initiated with clindamycin (600mg every 6 hours) and intravenous gentamicin (240mg every 24 hours) for 7 days. Although dysthermia was not documented during hospital stay, magnetic resonance imaging was performed, revealing uterus didelphys and hematocolpos (Figures 3 and 4).

Source: Document obtained during the study.
Figure 3 Magnetic resonance, coronal cut, that shows uterus didelphys, hematopyometra (A), hematocolpos (B) and their respective appendixes.

Source: Document obtained during the study.
Figure 4 Cross-sectional magnetic resonance showing two uterine bodies.
During hospital stay, the symptoms of the patient improved and pain resolved. Surgical management was proposed for marsupialization of the vaginal septum, but the patient and her relatives decided to dissent the procedure during hospitalization and expressed their desire to postpone it. Considering the resolution of the symptoms, hospital discharge was approved once the antibiotic management was completed without any further intervention.
Since the patient was referred to the hospital due to a company benefit plan that did not include outpatient consultation with the institution, it was not possible to perform institutional follow-up.
DISCUSSION
The reason why HWW syndrome presents with a higher prevalence of malformations on the right side as well as incomplete vaginal obstruction is unknown. These conditions, however, have an impact on the late diagnosis of complete vaginal obstruction, since the symptoms appear early in the latter category. 1
The possibility of diagnosing this syndrome cannot be ignored when a physician receives a patient with foul-smelling vaginal discharge, whether it is small or rare, because partial perforations in the vaginal septum lead to this scenario.
Regarding anatomical variations, it is possible to classify HWW syndrome according the presence or not of septum or cervical fistulas in: type I, the vaginal septum is not perforated (Figure 5); type II, septal perforation is observed (Figure 6); and type III, the vaginal septum is unperforated with cervical fistula (Figure 7). 2 In the light of this anatomical classification, it is understood that the definitive treatment is surgical correction, in which the vaginal septum obstructing the hemi-uterus is resected, thus allowing communication with the vaginal lumen.
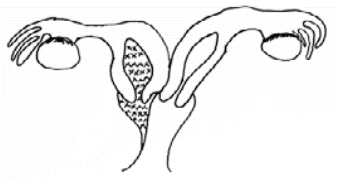
Source: Own elaboration.
Figure 5 Herlyn-Werner-Wünderlich syndrome type I: unperforated vaginal septum that favors hematometra and hematocolpos.

Source: Own elaboration.
Figure 6 Herlyn-Werner-Wünderlich syndrome type II: perforated vaginal septum that communicates the flow with the lumen of the permeable hemivagina.

Source: Own elaboration.
Figure 7 Herlyn-Werner-Wünderlich syndrome type II: vaginal septum without perforation that connects the cervix and allows cervix fistulization.
Pregnancies are more likely to occur in the uterus opposite to vaginal septation, although post-marsupialization increases the possibility of pregnancy on the side ipsilateral to renal agenesis. 2 The possibility of miscarriage is not ruled out; however, only 15% of patients with HWW syndrome present conceptional losses.
Patients with this pathology benefit from marsupialization of the septum that makes up the blind or fistulized vagina, in such a way that the menstrual content of the obstructed hemi-uterus is easily expelled from the cavity, thus preventing the formation of blood or hematopurulent collections.
With respect to female urogenital malformations, only 3.53% present the diagnostic triad of the HWW syndrome. 4 Another study reveals that 2-3% of the population with fertility problems have HWW syndrome and that only 0.3% of the general population suffer from this pathology. 5 1 in 2 000-28 000 women can develop this syndrome 6; the differences in frequency are explained by the iceberg theory, which would account for the disparate and unclear prevalence of the syndrome, since many patients are asymptomatic and others are underdiagnosed.
CONCLUSIONS
The HWW syndrome is a rare Müllerian malformation that can have a significant impact on the life of the patient who is suffering from this pathology, given that morphological changes make them more prone to consult for gynecological infectious diseases or blood collections (hematometra or hematocolpos). Definitive surgical management of vaginal septum improves the quality of life of patients and reduces the risk of morbidities associated with the pathology. Obstetric results are always linked to the implantation site of pregnancy.
Adequate articulation between the different networks of health service providers is required for better follow-up and adequate management of patients with HWW.
ETHICAL CONSIDERATIONS
It is hereby declared that the subject of this investigation, as well as her legal representative, participated voluntarily, following the principle of confidentiality, were aware of the possible risks or discomforts, and had the right to refuse or withdraw from the study.














