INTRODUCTION
Complex regional pain syndrome (CRPS) is a condition that affects 7% of patients with fractures and/or surgeries in the limbs or other injuries. Its clinical features include subacute, acute and chronic symptoms with autonomic and inflammatory characteristics. The condition of people with this syndrome improves within the first year, but in some patients, the disease progresses to its chronic form, usually in parallel with inflammatory symptoms, which prevail over autonomic ones. 1 CRPS is classified into two types: type 1, with no nerve damage, and type 2 (causalgia), with identifiable nerve damage. 2,3
CRPS manifests with localized pain associated with neuropathic pain (temperature changes, hyperalgesia and allodynia) and autonomic dysfunction (motor and sudomotor involvement). It may also be observed in regions distant from the site of injury. The etiology of this syndrome is not completely clear, although its physiopathology shows evidence of involvement at the central nervous system (CNS) and peripheral levels. 4
This case describes the clinical evolution of a patient who, after a trauma, presented neurological, vasomotor and inflammatory symptoms, which together are characteristic of CRPS. However, diagnosis was difficult to achieve because of the diversity of the symptoms; therefore, it was necessary to carry out personalized treatment according to the symptoms.
CASE PRESENTATION
A 21-year-old female patient, mestizo, unemployed, of a middle-income household and without significant medical history, attended the emergency service of a trauma center due to a trauma in the lumbosacral region secondary to a traffic accident (the woman was a passenger on a motorcycle when a car hit them from behind).
Physical examination showed pain and edema on palpation in the affected areas, so comparative hip scan and lumbosacral spine tomography were performed, obtaining normal results. The woman was assessed by the orthopedic and neurosurgical services, and single intravenous doses of dipyrone (2g) and tramadol (50mg) were administered for pain management. After this drug treatment, pain decreased and the patient was discharged.
One week later, the patient returned to the emergency department reporting intense pain (10 points on the pain scale) in the lumbosacral region associated with difficulty to sit. On physical examination, she presented edema, pain and decreased mobility of the arches. The woman was assessed by neurosurgery, which ordered lumbosacral spine tomography and lumbosacral spine nuclear magnetic resonance imaging (LSN-MRI), reaching a diagnosis of sacrococcygeal dislocation (Figure 1). She was discharged with orders for outpatient treatment with acetaminophen 500mg every 6 hours, diclofenac 100mg per day, and pregabalin 50mg every 12 hours, and instructions to sit on a flotation cushion.

Source: Document obtained during the study.
Figure 1 Lumbosacral spine CT showing sacrococcygeal dislocation.
Four weeks later, the patient returned to the emergency department due to further trauma to the coccygeal region while riding in a car; the woman reported severe pain in the lumbosacral region with inability to walk. Physical examination showed pain in lumbosacral spine region when moving the lower limbs, good capillary filling and absence of paresthesia in lower limbs. The patient was assessed by the neurosurgery service with new imaging that showed no changes; intravenous analgesic treatment was given: dexamethasone (8mg), tramadol (50 mg\mL) and dipyrone (2g). She was discharged based on the improvement of the symptomatology.
Six weeks later, the patient attended a follow-up appointment and reported referred pain in the sacrococcygeal region that radiated to the bilateral inguinal region when sitting down that became more acute when performing Valsalva's maneuvers. Symptoms were treated with amitriptyline (25mg every night), acetamin-ophen+codeine (500 mg\8mg every 8 hours) and bisacodyl (5mg every night) for constipation.
A follow-up appointment took place four weeks later, and the patient reported persistence of radicular pain in the coccygeal region, which intensified when sitting and walking, so a peridural block was indicated. Four weeks later, during a new follow-up appointment, the woman said that her symptoms improved only during the first two weeks after the procedure, and on physical examination she reported permanent pain in the coccygeal region with little tolerance to palpation, even in decubitus; consequently, the neurosurgery service indicated coccygectomy. Five days after the procedure, she presented radicular pain and limited mobility of the left leg irradiated to the ipsilateral ankle. Given the symptomatology, neuralgia was considered and treatment with pregabalin was initiated (150mg every 12 hours); the symptoms improved and she was discharged.
Fifteen days after the last discharge, the patient was readmitted to the emergency department for moderate bleeding on a surgical wound associated with general discomfort and chills. Physical examination revealed suture dehiscence, moderate bleeding, erythema, flushing and heat. The neurosurgery service performed a new assessment and indicated surgical washing and resuturing the wound; a culture was taken, and it was positive for Escherichia Coli, so 2g of cefazolin were administered every 8 hours. The patient presented monoparesis in the lower left limb during hospitalization, so a new LSNMRI was requested, yielding normal results.
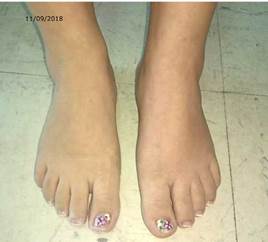
During the second week of hospitalization, the patient presented radicular pain in the lower left limb, minimal sensory changes in the left L5-S1 segment (partial objective difference in distal S1 strength and minimal difference in ipsilateral L5), sensory alteration of the lower left limb (from L5 to S1) and changes in temperature, hypostesia, allodynia and coloration in the dorsum of the left foot (Figure 2).
Considering the mechanism of trauma, the time of evolution of the patient, the type of injury and the symptomatology, it was concluded that the woman suffered from Type I CRPS (post-traumatic). Treatment was initiated with topical capsaicin, amitriptyline (25mg per day), prednisolone (15mg per day), pregabalin (150mg per day), acetaminophen (1 000g every 8 hours) and physical therapy. In addition, based on her limited mobility and frequent pain, the woman felt worried and depressed, so she required support from the psychology service, and accompaniment from her family group.
In the third week of her hospital stay, the symptoms improved; she was able to move around with the help of a walker and was subsequently discharged. Two weeks later, she attended a follow-up appointment, finding paresis (3/5) in the left crural nerve, paresthesia in the left L4-L5-S1 segment, and change of color and increased temperature in the distal region of the left lower limb. In addition, the surgical wound (sacrococcygeal region) showed severe discharge without signs of local infection associated with suture dehiscence. A pelvic MRI was performed showing surgical wound level collection with density of clear serous fluid (Figure 3).

Source: Document obtained during the study.
Figure 3 Pelvic MRI showing collection at the surgical wound site.
Assessment by plastic surgery was requested, reporting that the surgical wound was not deep enough to compromise vital structures and that, due to its location, expectant management was sufficient for closure by secondary intention. Finally, the patient began physical therapy treatment, recovering motor function. It should be noted that although the patient was treated with different medications, she had no side effects and had good adherence to the treatment.
DISCUSSION
The origin of the CRPS involves several aspects that must be taken into account to understand its complexity:
Inflammatory mechanisms
Cytokines and nerve growth factor (NGF) released after tissue trauma can stimulate nociceptors, leading to long-term peripheral sensitization. 5,6 The activation of primary nociceptors generates a retrograde depolarization of small diameter primary afferents (also known as axonal reflex) that release substance P (SP) and calcitonin gene-related peptide (CGRP) from the sensitive nerve endings of the skin. This process leads to vasodilation and protein extravasation in the tissue, and causes classic clinical signs of CRPS (redness, heating, edema). 7
In skin biopsy results, the levels of tumor necrosis factor a and interleukin-6 are higher in patients with CRPS than in those who are not affected, a difference that is solved within six years after the injury. 8 Pro-inflammatory cytokines are likely to act not only locally but also at the spinal cord -perhaps secondary to sensitization of nociceptive neurons or neuronal interaction-, leading to mechanical hyperalgesia. 9
Studies such as Blaes et al.10 and Kohr et al.11 establish that about 35% of CRPS patients generate surface binding autoantibodies against sympathetic and mesenteric plexus neurons. It is possible that the antigens of these auto-antibodies are adrenoreceptors a and acetylcholine muscarinic receptors. It should be noted that this is only one hypothesis which should be further studied, since patients have not presented, so far, generalized autonomic failure caused by the action of serum autoimmune antibodies.
Vasomotor dysfunction
With this type of dysfunction, patients feel that the affected limb is warmer or cooler compared to the opposite limb. Vasomotor dysfunction is more common than previously thought in patients with CRPS 12 and has three different presentations 13:
Hot/warm: the affected limb is warmer than the opposite limb, there are elevated norepinephrine levels in terms of venous circulation in the affected area, and it lasts an average of 6 months.
Intermediate: the affected limb may be warmer or cooler than the non-affected limb depending on sympathetic activity, and lasts an average of 5 months.
Cold/blue: the affected limb has decreased temperature and low norepinephrine levels compared to the opposite limb, which lasts for more than 6 months.
In summary, besides inflammatory vasodilation, there is also unilateral inhibition of cutaneous vasoconstrictive sympathetic neurons. This condition in the thermoregulatory system can be caused by functional changes triggered by the initial trauma to the spinal cord, brain stem, or brain.
Finally, in the chronic presentation of CRPS, altered neurovascular transmission and hyperreactivity of blood vessels to circulating catecholamines tend to prevail. It should be noted that not all patients with the syndrome present the characteristics mentioned above; for example, those who have the syndrome as a result of poor activity of cutaneous vasoconstrictive sympathetic neurons in nocireceptors develop sensitivity to catecholamines, which contributes to pain symptoms. 14,15
Central Nervous System (CNS)
In patients with CRPS, the CNS undergoes functional and structural changes that generate persistent pain and central sensitization, increasing the excitability of spinal cord neurons. 16 Sensitized spinal nociceptive neurons, on the other hand, are more receptive to the input of peripheral stimuli and can generate impulses in the absence of stimuli, resulting in chronic pain (which can sometimes radiate into nearby uninjured areas), hyperalgesia and allodynia. 16 Activation and regulation of glutamate receptors make signal transmission in the nociceptive circuit from the spinal cord to the cortex more effective. 17
It has been shown that patients with chronic CRPS perceive their affected limb to be longer than it actually is. (18) They also present distortions of the mental image of their limb (temperature and shape) and develop a feeling of hostility towards it. 19
Diagnosis
CRPS diagnosis is mainly clinical; it is based on the presence of symptoms and signs associated with the autonomic, motor and sensory disorders described above, and also on the Budapest criteria, which have a sensitivity of 85% and specificity of 69%. 20 In order to consider CRPS, the patient must have at least one of the signs from the four categories posed by these criteria.
Before determining that the patient suffers from CRPS, other pathologies must be ruled out, such as rheumatic diseases, arthritis, post-surgical infections, cellulitis, neuritis, neuralgia, thrombosis, compartment syndrome, among others. X-rays and bone scans are tests that help achieve the diagnosis. 21
Treatment
Patients with CRPS must have a positive and active attitude to achieve adequate rehabilitation in the shortest time possible. Regular physical and occupational therapy help reduce pain and motor impairment, especially in early presentations of the syndrome, and improves the coordination of the limb. 22 In some cases, transcutaneous electrical nerve stimulation, which is not tolerated by patients with allodynia and hyperalgesia, may be helpful for pain reduction therapy. In this sense, it is necessary to establish a personalized treatment for each patient according to their need. 23
Primary care for CRPS usually begins with non-steroidal anti-inflammatory drugs to slightly decrease pain; if the pain is neuropathic, gabapentin 24,25 and opioids show favorable results. 26
Opioids tend to be less effective for controlling chronic neuropathic pain compared to acute conditions. 27 In addition, they produce different side effects and can generate tolerance and hyperalgesia. 28 Therefore, when prescribing them to treat CRPS, it is important to consider that they reduce pain and can help improve the quality of life in some patients, but they can generate more pain and dysfunction in others. Intravenous administration of lidocaine is also effective to control neuropathic pain and CRPS 29 by reducing the degree of pain, whether spontaneous or evoked. 30
The treatment of CRPS has been studied by several authors, who argue that it can be managed using different drugs. Van Hilten et al.31 reported that baclofen helps improve associated dystonia; Adami et al.32 and Varenna et al.33 state that bisphosphonates are effective to control pain, swelling and mobility; Schwartzman et al.34 and Sigtermans et al.35 found that intravenous administration of ketamine significantly reduces pain scores and improves motor function, as allodynia in patients who received it showed significant improvement in the affected limb, turning it into a good therapeutic option. 36
Capsaicin is a topical treatment that can be useful in patients with CRPS as it potentiates the release and inhibits the reception of P substances from the afferent polymodal non-myelinated terminals; therefore, it has an analgesic effect on some presentations of neuropathic pain 37, although in some patients, it may produce a burning sensation that is difficult to tolerate. 38,39 This side effect can be so severe that a regional anesthetic block must be performed in order to continue treatment at high doses. 40
Some studies show a decrease in pain in patients with CRPS who undergo sympathectomy. 41,42 Other procedures that have proven to be effective to reduce pain and improve CRPS are spinal cord stimulation 43 and peripheral nerve stimulation. 44
In the clinical case presented here, this condition developed after receiving a trauma in a localized region, which was not severe nor compromised the quality of life of the patient at first, and then she experienced gradually a variety of non-specific, varied, irregular and recurrent symptoms (which became chronic). This meant that CRPS could only be diagnosed in the presence of inflammatory, vasomotor and neurological symptoms that led the treating physicians towards that diagnosis. Since the symptomatology did not improve, or partially improved, and new symptoms appeared, the therapeutic approach focused on improving the patient's quality of life and initiating early physical rehabilitation; however, this was not enough, so other therapeutic options had to be implemented (from blocks to coccygectomy). Unfortunately, these measures only led to a partial and short-lived improvement and then the symptoms worsened.
The clinical condition of this patient posed a great challenge for the treating physicians, so it was necessary to make a multidisciplinary therapeutic approach to improve her evolution. Thanks to that multidisciplinary work, the adherence to the treatment, the absence of side effects and the disposition and determination of the patient, her quality of life improved to the point of resuming a normal daily life.
CONCLUSIONS
This clinical case made evident that CRPS has a variety of non-specific symptoms that may become acute despite the treatment, and is therefore considered a difficult disease to diagnose.
Since the cause of this disease is multifactorial, a multidisciplinary therapeutic approach must be adopted, not only focusing on medical aspects, but also on psychological aspects in order to improve the quality of life of the patient and to enable him/her to return to his/her daily routine as soon as possible. Consequently, more efforts should be made to better understand the specific mechanism by which CRPS occurs and thus train medical personnel to initiate appropriate and timely multidisciplinary treatment.