INTRODUCTION
Pneumomediastinum, also known as mediastinal emphysema, is defined as the presence of air in the mediastinum. It can be secondary to surgery, visceral perforation, infection, or trauma, but it can also occur spontaneously and is known as spontaneous pneumomediastinum 1 or Hamman's syndrome. This entity is rarely observed in emergency departments. 2
This condition can be classified into two groups. On the one hand, spontaneous pneumomediastinum has no primary cause identified and, on the other, secondary pneumomediastinum has clear causes, such as penetrating trauma, closed chest trauma, recent interventions in the esophagus or tracheo-bronchial tree, pneumothorax, mediastinal or pulmonary infection by gas-producing germs, among others. 3
Spontaneous pneumomediastinum was first described in 1819 by Laenec 3, and refers to the spontaneous rupture of the alveolus in situations of increased alveolar pressure (coughing, vomiting or Valsalva maneuvers). One of its associated conditions is asthma, as the mediastinal cavity is bounded laterally by the pleura, the diaphragm at the lower level, and the thoracic inlet at the upper level.
Moreover, pneumopericardium is defined as the presence of air in the pericardial cavity. This is a rare complication and few cases related to asthma have been reported, since it is associated with mechanical ventilation in newborns and with iatrogeny, trauma, tumors, infections or idiopathic appearances in adults. This pathology, which can often coexist with pneumomediastinum, was first described by Bricketeau in 1844. He found a sign known as bruit de moulin, which is a sound similar to that produced by the blades of a mill when they hit the water. 4,5
A patient with pneumopericardium may present mediastinal tympanism, pulsus paradoxus, jugular vein distention and muffled heart sounds; in addition, electrocardiogram may show tachycardia and signs of pericarditis. Large pneumopericardium can produce cardiac tamponades that require early diagnosis and treatment, but these are mostly mild conditions that respond to supportive measures. 4,5
CASE PRESENTATION
A 17-year-old female student from Girón (Santander, Colombia; 777 m.a.s.l.), from a middle-class household, non-smoker, with a history of asthma diagnosed since childhood (age not specified) and without treatment, attended the emergency room after experiencing symptoms for 2 days. They included persistent cough with greenish expectoration, dyspnea, wheezing, chest tightness, cough associated with cyanosis, dysphagia, and chest pain radiating to the neck and shoulders.
Physical examination found: blood pressure: 122/82 mmHg, heart rate: 107 beats per minute, respiratory rate: 22 breaths per minute, oxygen saturation: 97% at room temperature, temperature: 36°C and wheezing in both lung fields. The patient also reported pain in the right supraclavicular region and anterior neck, and subcutaneous emphysema was found in the right supraclavicular region on palpation (Table 1).
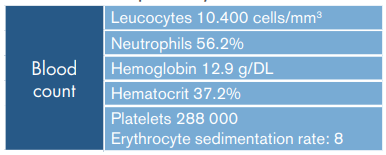
Table 1 Laboratory tests on admission.
| Leucocytes 17 200 cells/mm3 | |
| Blood count | Neutrophils 79.2% |
| Hemoglobin 15 g/DL | |
| Hematocrit 44.7% | |
| Platelets 367 000 | |
| Kidney | Creatinine 0.72 mg/dL |
| function | Urea Nitrogen 16.3 mg/dL |
| Arterial blood gas | pH: 7.458, PO2: 62.2, PCO2: 32.7, SatO2: 92.8% |
| HCO3: 22.6 mmol/L, BE: -0.4 mmol/ L | |
| Lactate | 1.72 mmol/L |
Source: Own elaboration.
Posteroanterior and lateral chest x-rays were taken, showing normal cardiac silhouette without pleural effusions or flattening of the diaphragm, but increased bronchovascular network without consolidation towards the lung bases and subcutaneous emphysema towards the right supraclavicular region with posible pneumomediastinum (Figure 1).

Source: Document obtained during the study.
Figure 1 Posteroanterior and lateral chest x-rays. => Subcutaneous emphysema in right supraclavicular region and air in mediastinum.
Since pain in the supraclavicular región and right anterior neck was persistent and pneumomediastinum was suspected, a computed tomography (CT) scan of the chest was indicated, confirming pneumomediastinum.
There, air was observed dissecting the mediastinal planes and the base of the neck, with extension to the supra scapular region on the right side; discrete pneumopericardium was also evident (Figure 2).

Source: Document obtained during the study.
Figure 2 CT Scan of the chest. => Pneumomediastinum and pneumopericardium.
Based on these findings, the patient was admitted to the hospital and advised to rest, receive oxygen by nasal cannula, respiratory therapy with bronchodilators (initially salbutamol and berodual through nebulization, and later salbutamol in spray by schedule), systemic corticoid (initially intravenous hydrocortisone and later oral prednisone), and 1.5g of intravenous ampicillin sulbactam every 6 hours.
The patient was assessed by the pneumology service, which considered that she was suffering from moderate asthma attacks, acute bronchitis with pneumomediastinum, and pneumopericardium. For this reason, bronchodilator and corticoid treatment was continued, and clarithromycin 500mg orally every 12 hours was added to the antibiotic treatment, which continued to be ampicillin sulbactam until completing 7 days. She had good adherence to treatment and showed no adverse reactions.
Finally, a follow-up chest x-ray showed normal cardiac silhouette with increased bronchovascular network without consolidation towards the bases; no pleural effusions or flattening of the diaphragm were found. The patient completed the antibiotic treatment established by pneumology with adequate clinical response, resolution of wheezing, improvement of dyspnea and absence of subcutaneous emphysema, so she was discharged with medical recommendations and warning signs.
DISCUSSION
Pneumomediastinum is a rare entity with a prevalence of 1 case per 7 000-44 000 hospital admissions. It is more frequently observed in young patients without comorbidities, with the exception of asthma, and more than 75% of the cases occur in males with an average age of 20. 6
Two incidence peaks have been reported in the pediatric population: in children under seven years of age, probably secondary to lower respiratory tract infections, and in adolescents, due to asthma attacks and upper respiratory tract infections. 7 The increase in intrathoracic pressure is the main predisposing factor: the rupture of the alveoli, secondary to a difference in pressure gradients between the alveoli and the mediastinum, moves the air from the place with the highest pressure gradient (intra-alveolar space) to the mediastinal structures with the lowest pressure gradient. 8 The dissection to release the free air is not only limited to the mediastinum, as this communicates with the mandibular space, the retropharyngeal space and the vascular beds within the neck. Once in the mediastinum, air can flow and cause pneumoperitoneum, pneumothorax and subcutaneous emphysema, although free air has also been found in the peritoneum, causing pneumoperitoneum. 1,9
Regarding severe asthma, pneumomediastinum develops due to the over-expansion of the distal airways caused by bronchial obstruction with subsequent alveolar rupture. The most common symptoms described in the literature are dyspnea and chest and neck pain. 10,11 Chest pain is acute, retrosternal and pleuritic, and may radiate to the neck, dorsal region or shoulders. 10 Neck edema and odynophagia have also been reported and, on physical examination, neck skin crackles are palpated, a finding consistent with subcutaneous emphysema. 11
Rarely, voice changes and dysphagia may be observed, which are secondary to the displacement, usually anterior, of the larynx and esophagus by the air present between the fascias. 12 The accumulation of air between the anterior parietal pericardium and the underlying chest wall can produce a crackling in the precordium region, which is synchronized with heart sounds. 10,12 In the case presented here, the patient's symptoms coincided with the literature, which reports that this pathology can occur in asthmatic patients, generally in contexts of exacerbation of respiratory symptoms. Clinically, there are no signs that allow associating pneumopericardium with asthma.
Patients with suspected pneumomediastinum diagnosis should undergo anteroposterior and lateral chest x-ray that includes the cervical area. 3 Confirmatory imaging findings include signet ring sign around the artery, double bronchial wall sign, continuous diaphragm sign, thymic sail sign, and subcutaneous emphysema. 3,8 The results of this test are usually normal in 10-30% of patients, especially in supine projection. 3
If the x-ray does not provide information, the chest CT will lead to the diagnosis, as it has been shown to be superior to x-ray in locating and measuring the extent; it is also important for differential diagnosis. 6,8 In this case, the disease was confirmed based on the images, which showed pneumopericardium, although no clinical sign had been reported.
In general, pneumomediastinum is benign and has good prognosis 1; its treatment is usually conservative, based on pain management, rest and bronchodilators. In addition, Valsalva maneuvers should be avoided and sometimes antibiotics and oxygen are necessary 6,10, reaching clinical resolution around the fourth day. 8 Pneumopericardium may resolve spontaneously, but in some cases pericardial drainage is necessary, especially with signs of tamponade. 5
The differential diagnosis of spontaneous pneumomediastinum includes pneumothorax, pulmonary embolism, pericarditis, tracheobronchial tree rupture and Boerhaave syndrome (retrosternal chest pain and subcutaneous emphysema in the neck after vomiting). 12
CONCLUSION
Spontaneous pneumomediastinum is a rare condition that has signs and symptoms that may suggest several diagnostic options, ranging from general respiratory symptoms to precordium pain and subcutaneous emphysema. With respect to pneumopericardium, clinical findings include mediastinal tympanism, pulsus paradoxus, jugular vein distention or alterations perceived during auscultation, findings that are not always present, making clinical suspicion and diagnostic guidance vital to reach an effective treatment. Therefore, imaging is fundamental; the imaging method of choice is chest X-ray, although, in the event of normal findings and high clinical suspicion, a chest CT should be performed.
The evolution of pneumomediastinum is generally benign and associated with a good prognosis, but taking into account that it is rare, it is important to rule out other pathologies that may trigger an unfavorable outcome in the patient.
ETHICAL CONSIDERATIONS
The authors state that no human or animal experiments were conducted for this research and that the workplace protocols on patient information management were followed.
This case report was approved by the ethics committee of Los Comuneros Hospital Universitario de Bucaramanga S.A., by means of an unnumbered document dated May 22, 2018. The patient's mother authorized its publication in writing.